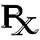Science-Based Medicine
Are there any real alternatives?
UPDATED: April 12, 2026
Welcome to the Healthy Living Is Good Medicine Newsletter, presenting timely, science-based, original articles covering a wide range of preventive medicine and public health topics, along with critical commentaries on the politics and economics of the American healthcare system.
Bottom Line, Up Front
There is only one kind of science-based medicine. It’s not perfect, but it does focus on the root causes of illness and preventing disease, deals with the whole person, is monitored for safety and effectiveness, and is constantly striving for measurable results. Everything else that’s being marketed as “alternative medicine” isn’t medicine. Those alternatives often involve some degree of quackery, with the promotion of uninformed, unproven, or even fraudulent “healing” practices, primarily for personal gain.
In most parts of the world, the need for qualified healthcare personnel exceeds the supply, creating opportunities for scammers. In America, the takeover of medical services by profit-driven corporations has created a flawed healthcare delivery system that is unable to provide universal accessibility and affordability.
Don’t confuse the American healthcare system with conventional medicine’s science-based approach to the diagnosis and treatment of illnesses and injuries. While far from being perfect, it’s not the occasional failures to cure by modern medicine that makes many people seek non-medical alternatives for their health problems. In large part, it’s that the for-profit delivery and payment systems often fail to meet people’s legitimate needs for affordable and accessible medical care.
About Science
Scientific facts are defined as independently verifiable observations made by qualified observers. Although observation techniques may need to be refined, and interpretations of the factual data can vary, there are no legitimate “alternate facts.” While scientific research is far more nuanced than I can go into here, suffice it to say that reputable scientists will typically agree about the facts, but may still debate the conclusions that are drawn from them. Those lively debates over interpretations are one of the many ways in which scientific knowledge advances.
Because of science’s data-gathering precision and its rigorous testing of provisional conclusions, any healing practices that are marketed as alternatives to science-based medicine should be viewed with skepticism. What’s scary is that the umbrella term, “alternative medicine,” provides cover for a broad assortment of charlatans, grifters, con artists, scammers, and misguided or poorly educated practitioners.
Unscrupulous professionals and “wellness” hucksters frequently exploit the flawed argument that something is inherently good because it is “natural,” or bad because it is “artificial.” Those claims ignore the many things found in nature that are harmful, and the abundance of manufactured things that are very beneficial.
Strange Beginnings
My interest in preventive medicine was partly influenced by the hippie, counterculture, and New Age movements of the 1970s. That led me to explore many so-called “natural healing” modalities early in my medical career. I joined the American Holistic Medical Association (AHMA), and was invited to lecture at a prominent naturopathic college.
As a result, I became very familiar with the whole gamut of pseudoscientific “alternative” (ie. non-medical) approaches to healing. I studied acupuncture, homeopathy, herbal medicine, hypnotherapy, and therapeutic touch. After recognizing the many limitations of these alternatives, along with their frequent therapeutic failures and occasional inexplicable successes, this “prodigal son” returned to the fold of conventional, science-based medicine.
Preventive Medicine
As one of my readers noted, “An ounce of prevention beats a pound of pills, but when prevention isn’t enough, thank goodness for the pills.” I’m still a strong advocate for preventive medicine and healthy lifestyles, but when lifestyle interventions such as a healthier diet, more physical activity, better sleep, stress-reduction, and so on aren’t effective enough, I’m quite happy to offer prescription medications that have a good track record for safety and effectiveness.
I realize that my profession needs to earn the public’s trust, and doctors who lack competence and/or scruples need to be weeded out. I can understand people’s wariness when conventional medicine hasn’t helped them, but that’s not a good reason for patients to see glorified vitamin salespersons with medical degrees. Let the consumer beware, and be on high alert for grift when a doctor deviates from the standard of practice for their medical community.
On top of that, there is a systemic problem with America’s for-profit healthcare model. Our Wall Street overlords make bigger profits by overworking healthcare providers employed by the corporations they own. For-profit health services are typically owned by private equity firms or are publicly traded. Insurance companies rake in billions in profits by raising healthcare premiums and denying services. Everyone but the stockholders and company executives suffer the consequences. Every other country in the world has figured out how to make healthcare widely available and affordable for almost everyone.
Interestingly, the Caduceus pictured above, with two snakes intertwined around a winged staff, does not historically belong to medicine. Linked to Hermes, the Greek messenger god, it is a symbol of commerce. The Staff of Hermes represents travel, trade, business negotiations, and sometimes trickery and thievery. Perhaps that’s a more apt symbol for the highly profitable business of healthcare in the United States.
The Rod of Asclepius, depicting a single snake wrapped around a plain staff, is associated with the Greek god of medicine and healing, and son of Apollo. It is the historically correct symbol representing medicine, the healing arts, and the healthcare professions. The Rod of Asclepius has been adopted as a logo by many international medical associations and public health organizations.
Despite all of its limitations, and the misdeeds of some of its practitioners, mainstream medical practice still offers people a far better therapeutic armamentarium with more predictable treatment outcomes. Sadly, the hucksterism that eventually infected the holistic, integrative, and functional approaches to healing has undergone multiple incarnations, and is now infesting broad reaches of American society in MAHA guises. With so many “doctor” choices, it is becoming increasingly difficult to choose appropriate healthcare providers.
Functional Medicine
Functional Medicine (FM), as practiced by MDs and DOs, has not been standardized, is not a recognized medical specialty, and has no board certification. Its marketing appeal is claims of an individualized and broader, multifaceted perspective that focuses upon the underlying causes of chronic illnesses. FM does not have convincing scientific studies demonstrating that its methods are superior to standard medical care.
As the latest, pseudoscientific rebranding of Integrative Medicine, Functional Medicine is typically practiced with a religious zeal. Its practitioners promote extensive testing by non-mainstream laboratories, dispense dietary supplements and herbal remedies, prescribe and administer proprietary medications from compounding pharmacies or imported products that don’t have FDA approval. Treatments are typically far more expensive, and often not covered by insurance. They might even recommend raw milk.
It has been said that Functional Medicine is the ultimate misnomer, and it is certainly not the “new paradigm” in medicine. Anything that might be good about it is not unique to FM, and what is unique about it is most likely not good. That’s why I highly recommend conventional Western allopathic medicine, where established standards of care and specialty board guidelines give patients far greater protection and legal recourse when they are preyed upon by unscrupulous practitioners.
When seeking medical care, it is important to always verify credentials, search for medical board complaints and disciplinary actions, and avoid practitioners whose recommendations and methods clearly deviate from those that are generally accepted by their local medical community.
Vitamin salespersons with medical degrees, such as Mark Hyman and Casey Means, haven’t found a dietary supplement that they didn’t like. Functional medicine has become yet another way to tempt both patients and healthcare providers into the murky realm of alternatives to evidence-based medicine. Selling supplements and other unproven treatments to patients is obviously a financial conflict of interest, but it can become a huge cash cow for unethical practitioners.
Allopathic Medicine
“Medicine” in common parlance today refers to orthodox Western medicine. In the 21st century, the practice of conventional or allopathic medicine is science-based, and its healing arts have been supplanted by the engineering marvels of medical technology and high-powered computers. It did not surprise me that after practicing for a few years, a number of my naturopathic students wanted to offer patients the best that science can provide, and eventually went to medical school. The most important principle of conventional medicine is “First, do no harm!”
I shudder to think what would happen if “alternative medicine” became commonplace in hospital emergency departments. Aromatherapy for head trauma? Crystals for fracured limbs? Megavitamin infusions for cardiac arrest? Ivermectin for COVID-19? Prescribing private label herbs and dietary supplements, along with empty promises of greater longevity, is downright dangerous.
A 2026 cohort study of a dataset from the National Cancer Database that included female patients with breast cancer found that the use of alternative treatments instead of traditional therapies (such as surgery, chemotherapy, endocrine therapy, and radiation) was was associated with a 3.7 times higher mortality rate, which was similar to patients who chose not to be treated at all. The use of so-called complementary therapies, in conjunction with standard treatments, was linked to a 40% higher chance of dying within five years.
Alternative Medicine
While overseeing a multidisciplinary orthopedic rehabilitation facility, I was in contact with several surgeons, plus a chiropractor, naturopath, massage therapist, clinical psychologist, acupuncturist, and physical therapist. We were all committed to “staying in our own lane” while allowing patients to make empowering choices about their treatments. With weekly monitoring of patient progress, I had to evaluate if the “alternative” treatments were actually providing benefits.
The problems that I encountered with non-medical treatments was their lack of strict professional standards and absence of licensing agency oversight. That kind of laxity can enable unscrupulous practitioners to take advantage of gullible patients. For example, unethical naturopaths can easily get away with selling supplements and performing treatments of dubious quality and without any legitimate medical necessity. Chiropractors who don’t stick to spinal manipulation, and massage therapists who don’t stick to massage, might dispense unqualified medical advice or make recommendations tainted by conflicts of interest.
Whenever they are not required to have convincing scientific evidence for effectiveness and safety, charlatans of various stripes can get away with charging patients for worthless or even dangerous treatments. The entire seven trillion dollar “Wellness Industry” is basically a scam. Among its bogus claims are the so-called treatments for autism that have recently been endorsed by the deplorable MAHA huckster at the helm of the U.S. Department of Health and Human Services (HHS).
During his confirmation hearings for HHS Secretary, anti-vaccine activist and conspiracy theorist RFK Jr. repeatedly assured Congress that he wouldn’t take vaccines away from anyone. Instead, he devised an evil scheme to do exactly that by removing liability protections from vaccine manufacturers. Cutting into their profitability with a deluge of capricious lawsuits would discourage pharmaceutical companies from manufacturing vaccines and sabotage their vaccine research programs.
As a patient advocate, I have had to become a whistle-blower whenever I learned that medical doctors were ripping off their patients or acting unethically. That was only possible because my profession has very strict and clearly defined standards of practice, especially when compared to the other professions that I’ve mentioned. Being familiar with those standards made it easier for me to recognize violations, but who is looking out for the “alternative medicine” patients?
When an approach to treating illness is unsupported by bonafide scientific research and is employed instead of conventional medical diagnosis and/or treatment, it is typically labeled as “alternative medicine” by its practitioners. That’s a deceptive misnomer, akin to calling falsehoods “alternative facts.” Typically, those treatments have little in common with conventional medicine.
Employing treatments without convincing evidence for their safety and effectiveness, the potential dangers are multiplied when worthless treatments prevent patients from receiving a legitimate medical diagnosis and an appropriate treatment for their condition, delivered in a timely fashion.
Alternative practitioners will frequently rely upon their own “intuitive” diagnostic methods, such as dowsing, aura-reading, and muscle-testing. They might employ mysterious “energy healing” or “chakra-balancing” techniques, and prescribe vitamins, minerals, herbs, and dietary supplements that are misleadingly referred to as “nutraceuticals.”
Determining whether herbs, vitamins, and other over-the-counter dietary supplements would be helpful or harmful to you can be quite challenging. Memorial Sloan Kettering Cancer Center’s About Herbs database is a tool for both the public and healthcare professionals. It can help you determine the value of using common herbs and other dietary supplements.
Practitioners of alternative treatments have become quite adept at cashing in on the human body’s tendency to heal itself. Their ability to exploit people’s credulity is exemplified by a $5.6 trillion unregulated wellness industry.
For example, an alternative treatment consisting of coffee enemas has been promoted for “colon cleansing.” However, taking coffee up the butt has absolutely no proven benefits, and comes with the risk of serious side effects, including rectal burns and electrolyte imbalances.
Without effects that are significantly different from plain water enemas, when administered to randomly selected participants in a double-blind clinical trial, any health claims for coffee enemas must be considered doubtful. When they are employed at the Gerson Institute in Tijuana, Mexico, as part of its cancer treatment program, they represent dangerous quackery.
Becoming ever more creative in their strategies to avoid consumer protection measures and government regulatory oversight, the wellness industry has come up with another scam to separate the gullible from their money: IV Hydration Spas.
Alternative treatments usually come with false claims about being able to achieve the same results as conventional medicine, despite lacking biological plausibility, testability, repeatability, and convincing clinical evidence for effectiveness. While people have a right to their own opinion, they don’t have a right to their own facts, which are independently verifiable by qualified experts who strive for objectivity.
Be very skeptical about treatments that do not meet the standards of orthodox medical care. As Carl Sagan famously remarked, “Extraordinary claims require extraordinary evidence.” You simply won’t find that kind of evidence for alternative treatments, or they would have become part of mainstream medicine’s therapeutic arsenal.
When it comes to the wackiest alternatives to science-based medicine, “homeopathic remedies” are top contenders for the woo-woo prize. They defy logic and lack credible evidence for having anything more going for them besides a placebo effect. Homeopathy’s persistent popularity, explored in a recent article, simply boggles the professionally skeptical mind.
People who go down the alternative path will usually fare worse than those who receive no treatment at all, and the high out-of-pocket costs will add insult to their injury. Apple Computer founder, Steve Jobs, “trusted his intuition” rather than sound medical advice, and delayed potentially life-saving surgery in favor of alternative treatments. That enabled his cancer to advance until it became incurable.
I have had patients who would likely have gone into remission with standard cancer treatments if instituted early enough, but died as a result of pursuing alternatives. It is very disheartening to see patients when it is too late to help them. Even when conventional medicine can’t produce a cure, it can usually extend a person’s life and perhaps improve the quality of their remaining time. Dr. Wilson explains how cancer deaths are higher for people receiving alternative treatments, even when in conjunction with standard therapy:
Complementary Treatments
In contrast to alternative treatments, these treatments are relatively benign accompaniments to standard medical care, even though they don’t have a strong evidentiary basis for their efficacy. Examples include guided imagery and yoga for patients undergoing cancer chemotherapy, or acupuncture and massage for pain management, when used as an adjunct to doctor-prescribed medical care.
The argument for complementary treatments is that as long as they cause no demonstrable harm, they can potentially have a beneficial effect, even if it is only a placebo effect. That argument might have been more persuasive a half-century ago, when far fewer treatment options were available to physicians. Back then, the practice of medicine was not as well-guided by science as it is today.
The default position for modern medicine is “Show me the evidence!” If a treatment isn’t backed by convincing evidence, ethical physicians should not be employing or recommending it. The National Institutes of Health (NIH) currently maintains a National Center for Complementary and Integrative Health (NCCIH) where people can learn about a variety of non-mainstream treatments to help them make informed choices.
Integrative Medicine
In its best expression, integrative medicine (IM) combines conventional medical treatments with only those complementary practices that are supported by sufficient evidence for safety and efficacy. There aren’t a great many of those. Sadly, IM has opened the door to “complementary and alternative medicine” (CAM) with all its attendant pseudoscience and questionable practices, and has acquired the status of a medical specialty in the United States.
Many of the clinics run by for-profit healthcare corporations are now offering IM or a variant thereof because that’s what a lot of misinformed people want. If they didn’t have an integrative or complementary medicine program, they’d be losing patients, and the accompanying revenue.
In contrast to IM and its different incarnations, psychosomatic medicine actually deals with the diagnosis and treatment of patients who have complex body-mind problems. This can be done by coordinating the participation of a number of diverse medical specialties. This approach has been particularly helpful in the management of chronic pain conditions and stress-related disorders.
As for Chinese and Ayurvedic traditional healing practices, how good can they really be if they haven’t changed much in a thousand years? Their most valuable contribution to Western medicine has been their perspective on treating the patient as a whole person, rather than narrowly focusing on the disease itself. This is known as a “holistic” approach to healing. The most effective primary care providers could be those who’ve adopted a whole-person strategy for their practice, according to a recent pilot program.
Standards for Ethical Medical Practice
There are very good reasons for upholding the highest standards for medical care; people’s lives and wellbeing depend on it. Medicine’s primary dictum is, “First, do no harm.” The ethical practice of modern medicine involves adhering to the standards established by one’s medical community and maintaining competence through continuing education. Then, there are those unscrupulous practitioners who reject science-based medicine.
It saddens me to say that some members of the medical profession are burned out or no longer have their heads in the game. Even worse are those who are deliberately unscrupulous or downright dangerous, especially when they put profits ahead patients, or promote bogus treatments. According to a recent article, a new hoax called “cancer immunotherapy” has proliferated among the quack clinics in Mexico.
Keep in mind that anecdotal evidence is not scientific evidence, and should therefore be ignored, regardless of how appealing the advertising. One need look no further than Prevagen commercials to know what I’m talking about. Neither should you be persuaded by friends who “knew someone who was helped.” No amount of glowing testimonials or sloppy clinical trials can take the place of well-done, peer-reviewed, randomized controlled trials (RCTs) that strongly indicate a causal relationship between a medical intervention and its outcome.
Stem cell clinics in the U.S. are raking in fortunes by administering unproven treatments, according to a 2019 report. Such clinics may provide misleading information, or advertise that they are running clinical trials. However, these clinics almost always work without FDA regulatory approval and oversight, and do not follow legitimate clinical trial protocols. Treatment at these unregulated stem cell clinics also carries significant risks, according to a report by Science, Health, and Public Trust.
The Quackwatch website has a search engine that can help consumers identify health frauds and medical practitioners involved in shady practices, such as claiming they have an unconventional cure for cancer or Alzheimer’s dementia. Let’s not forget about all the greedy physicians who were complicit in the opioid crisis by prescribing Purdue Pharma’s OxyContin without a legitimate medical purpose.
Even common medical treatments and procedures can be over-prescribed and over-used. The most frequent example is when doctors prescribe antibiotics for virus infections, just because that’s what patients want or expect. Besides being ineffective, they pose a risk for encouraging the emergence of drug-resistant bacteria. Sadly, in this era of rating everything and everyone online, physicians who appropriately use antibiotics tend to get lower patient ratings.
Another example is when doctors have a financial incentive for performing a procedure, without clear evidence that it is significantly more effective than a less invasive approach. This has been the case with some interventional cardiologists who are placing too many coronary artery stents, which will then require patients to take expensive anticoagulant medications for the rest of their lives.
Even worse are the bad actors in the medical profession who cater to the weaknesses of famous people and ply them with drugs that eventually lead to their death. When Elvis Presley died, 14 drugs were found in his blood, including nearly toxic levels of codeine and morphine. Prince died from a fentanyl overdose, illegally prescribed by his doctor. Michael Jackson’s personal physician was found guilty of involuntary manslaughter for administering a lethal combination of sedatives and the anesthetic, propofol. Two doctors were recently charged in connection with the ketamine-related death of “Friends” actor Matthew Perry.
Covid Scams
Schemes and scams proliferated during the height of the coronavirus pandemic, and continue today. There are still some doctors still prescribing ivermectin for patients with COVID-19, despite an overwhelming number of well-conducted RCTs showing that ivermectin is ineffective against the virus. The anti-medicine FLCCC is still promoting bogus covid and cancer treatments, and Florida’s Surgeon General is still dispensing dangerous misinformation. There really aren’t “two sides to an issue” when the science shows that one side is clearly wrong.
The FDA has only approved ivermectin for human use in the treatment of some parasitic infections. It remains primarily a veterinary medicine. The FDA does not have regulatory authority over the prescribing practices of physicians, but it recognizes that “off-label use” of medications does occur. However, the FDA advises patients not to use ivermectin to treat or prevent COVID-19.
It is up to state licensing boards to discipline doctors who deviate from medical standards. This usually doesn’t happen unless patients file complaints with the medical board and an investigation is instigated. The California Medical Board issued a blanket warning in 2022, stating that doctors who prescribe ivermectin for COVID-19 may be subject to disciplinary action. Unfortunately, many other states are apparently less protective of patients.
If a patient suffers complications from a bout of COVID-19, such as having to be hospitalized, or the develop post-acute sequelae (aka Long-COVID), because their doctor prescribed ivermectin instead of Paxlovid, the doctor can be sued for malpractice. Deviation from the accepted “standard of care” is prima facia evidence of malpractice. It is then up to the patient’s attorneys to prove damages and obtain recompense.
Avoiding Medical Misinformation
Because it has become quite challenging to find reliable sources of medical information and evidence-based healthcare on the Internet, the National Institutes of Health (NIH) has created a guide for navigating online resources. Doing your own online research is complicated and has many pitfalls. It is safer to follow in the footsteps of people who have proven themselves to be trustworthy, such as Dr. Wilson’s “Methods Man Blog.” Here’s a handy guide for navigating your way through the minefield of medical misinformation.
Stick to trustworthy websites provided by the NIH, CDC, KFF Health News, the Mayo and Cleveland clinics and the like, and academic institutions that provide medical education. National advocacy organizations, such as the American Diabetes Association, American Lung Association, American Heart Association, and Alzheimer’s Association, have helpful patient guides.
You certainly won’t find reliable, science-based health information coming from the wellness industry and its purveyors. Don’t fall for the click-bait headlines that are actually a misreporting of legitimate scientific research, such as those that screamed about a direct causal link between COVID-19 vaccination and excess mortality.
What you don’t want to do is rely upon information sent to you by your “Facebook Friend.” It is more than likely to be wrong, unless they can back it up with references from reliable sources. Even then, there are a lot of untrustworthy studies published in journals that lack editorial scrutiny and peer review. Knowing what research you can trust is fairly complicated, but this article can help.
Social media algorithms are designed to promote emotionally-laden controversies and lead viewers down “rabbit holes” in which they become increasingly engaged with content that is similar to what they already believe. Confirmation bias then leads users into “echo chambers” where the false or misleading information can be reinforced.
While YouTube videos are a great resource for learning how to fix common plumbing problems, they are NOT the place to obtain medical advice, unless it is coming from a highly reputable source. Although I strive for accuracy and may update my Posts with new information when it becomes available, healthy skepticism and independent verification are encouraged. To assist readers with fact-checking, I’ll often include links to my sources.
Social media employs a number of “brain hacks” to exploit people’s inherent cognitive biases. When viewers are hooked on their preferred content, they become more likely to abandon critical thinking skills and be persuaded by conspiracy theories, much to their social and emotional detriment. The U.S, public school system has failed body when it comes to teaching children vital critical thinking skills, unlike world-leading Finland:
Medical Misinformation Kills
In June, 2019, anti-vaccine activist Robert F. Kennedy Jr. visited Samoa and met with local activists, stoking vaccine hesitancy and promoting falsehoods about vaccination causing autism. In October, 2019, Samoa experienced a measles outbreak.
In mid-November, a state of emergency was declared, and Kennedy wrote the Prime Minister, urging him not to employ vaccine mandates. Samoa’s health emergency lasted through the end of 2019, ending when 94 percent of the people had been vaccinated, providing the population with herd immunity.
By the time the outbreak was over, 5,697 people had been infected, and 83 had died, most of them children under five years of age. Complications of measles infections, which can include permanent hearing, vision, and cognitive impairments, are still having an impact.
It appears that Kennedy contributed to the public’s doubts about the safety and effectiveness of measles vaccination. In all fairness, correlation should not be interpreted as causation. However, the Samoan measles catastrophe has been frequently cited as a cautionary tale about the dangers of medical misinformation. The reality is that vaccination is medical science’s greatest achievement.
Despite his potential complicity in the Samoa tragedy, RFK Jr. is now Secreatay of the U.S. Department of Health and Human Services (HHS) under the Trump administration. Putting an anti-vaxer who has no medical or scientific qualifications in charge of our nation’s health seems like a crazy idea to me. It’s like having a fox guard a hen house.
Making matters worse, Dr. Mehmet Oz now heads the Centers for Medicare and Medicaid Services (CMS). Characterized as a “quack grifter” by physicians and nurses associations, Oz hawked dubious medical treatments and products on his former TV show. During the height of the COVID-19 pandemic, he pushed government officials to make hydroxychloroquine widely available, despite the absence of scientific evidence supporting its safety and effectiveness for that purpose.
Who to Trust
As always, “caveat emptor” applies when receiving medical advice from your friendly neighborhood naturopath, chiropractor, acupuncturist, or massage therapist, because they are NOT medical doctors, and they don’t have to adhere to the same high standards applied to those who have a medical license. This warning applies in spades to any medical information online that’s not coming from reputable journals.
Patients need to distinguish between bonafide experts and a plethora of charlatans, frauds, hucksters, scammers, and quacks. The first clue is in how health recommendations are presented. If results are guaranteed, watch out. Science-based medicine does not claim certainty. Science can only provide percentages and probabilities that help doctors make informed guesses about the most likely diagnosis and its appropriate treatment. Most of the time, their chance of guessing correctly is very high, but sometimes it is not.
A physician’s assessment will depend upon the totality of the information available to them at any given time. New information is constantly being published, but they might not yet be aware of it. If this sounds like doctors need to hedge their bets when diagnosing and prescribing, that’s actually what they do. Medical science depends upon population-based studies and statistical probabilities that must then be applied to unique individuals.
Most people are uncomfortable with uncertainty, especially when they are dealing with troubling symptoms or facing the prospect of a scary diagnosis or prognosis. We naturally want to feel sure that what our doctor is telling us is correct. Most doctors project a comforting sense of self-confidence when interacting with their patients. However, when a doctor presents their professional opinion, they are actually sharing their best guesses.
It may be troubling for you to read this, but it is important to understand the limitations of medical science, as well as its truly amazing accomplishments. Having a realistic picture enables people to avoid becoming enthralled by alternative practitioners, whose stock in trade is holding out false hopes and making impossible claims. People want to believe in the promise of a cure. Sad to say, there are also unethical medical doctors who enrich themselves by taking advantage of their patents’ psychological vulnerabilities.
It never ceases to amaze me how many people fall for misleading claims and false promises, and how easily they can be manipulated and exploited by con artists in a variety of guises, be they political, religious, financial, or medical. I’m not just talking about “crystal energy” healers or “aura-balancing” practitioners, with no legitimate basis for their claims. I’m talking about anyone who is trying to sell you on something, including your friends. For example, the multi-level marketing (MLM) of “nutraceuticals” and hyped-up “alkalinizing” devices that claim to modify your drinking water in order to make your body less acidic. I recommend that you categorically reject all MLM products, regardless of who is selling them.
The bulk of the vitamin, supplement, and herbal medicine industries, and most of those who prescribe these unregulated products, are only trying to separate people from their money. The pharmaceutical industry is not beyond reproach on this account, either. Have you seen all the drug commercials on TV? If a medicine has a good track record, your doctor will already know about it, and you won’t have to ask them if it is right for you. Bottom line: If something sounds too good to be true, be very wary of it.
A New Paradigm for Medicine
The treatment and prevention of chronic illnesses is undergoing a rapid paradigm shift that involves seeing the body not as a machine with failing parts, but rather as a complex, interconnected, potentially self-repairing ecosystem that has gotten out of balance. Analogous to an old-growth pine forest with an infestation of bark beetles due to climate change, the system needs to be addressed as an integrated whole.
The AI technology employed for graphing neural networks can analyze multi-dimensional data streams and their interconnections, which can then be used to predict potential problems and develop personalized, integrated, and participatory interventions. Dr. Stickler explains the ecology of health and the network approach to future medicine in detail:
Conclusion
The alternatives to objectively verifiable facts are superstitions, unfounded beliefs, and manipulative fabrications. The alternatives to science-based medicine mostly consist of placebos, wishful thinking, and bogus “cures” that lack independent oversight and can be downright dangerous.
Anyone offering healthcare or health advice is urged to follow medicine’s prime dictum: “First, do no harm.” Please recognize that great harm can result from delaying legitimate medical diagnosis and treatment. Conventional Western medicine, like democracy, isn't perfect, but when it comes to life-saving interventions, it's the best we have.
Being human, medical doctors make mistakes, but they are still able to help most of their patients, most of the time. The best of them are in very short supply. Rest assured that when it comes to dealing with specific illnesses, there are no healthcare practitioners more qualified than those with an MD or DO after their name, provided they adhere to ethical practices and follow the medical standards established by their specialty.
I urge you to let your critical thinking guide your choices, rather than making emotion-based decisions. Understand and follow the science, and don’t let yourself be taken in by woo-woo and quackery. If you want a massage for aching muscles, or a spinal manipulation for a crick in your neck, that's fine. Just be sure to seek out licensed professionals, and check with their licensing boards for any complaints against them.
America’s profit-driven healthcare system is badly flawed, but people from Canada who can afford to do so come here for specialized medical treatment. Your best bet is to become an informed patient, so you can actively collaborate with your own doctor in formulating your care plan, rather than simply being a passive healthcare consumer. Protect yourself by becoming science literate, and learn from those who respect the science of medicine.
This Post may be updated at any time. Please check back here again to find the most up-to-date information on this subject.
You can find more articles about Healthy Living in my Post Archive.
You can help your friends and followers become healthier by suggesting that they subscribe to this Newsletter. You may receive access to premium features as a thank-you for making referrals:
If you find this Newsletter to be of value, and would like to lend your support, become a paid subscriber or make a donation. That will prompt Substack to promote this publication and help it reach many more people.